|
I read the other day on social media a suggestion for patients when selecting a healthcare provider to ask them their definition of pain to see if it is similar to the definition provided by the International Association of the Study of Pain (IASP).
Interesting idea. The key for me is if they understand pain is biopsychosocial (BPS) in nature and treat it that way. I may have to ask this going forward. What do you think? Related information
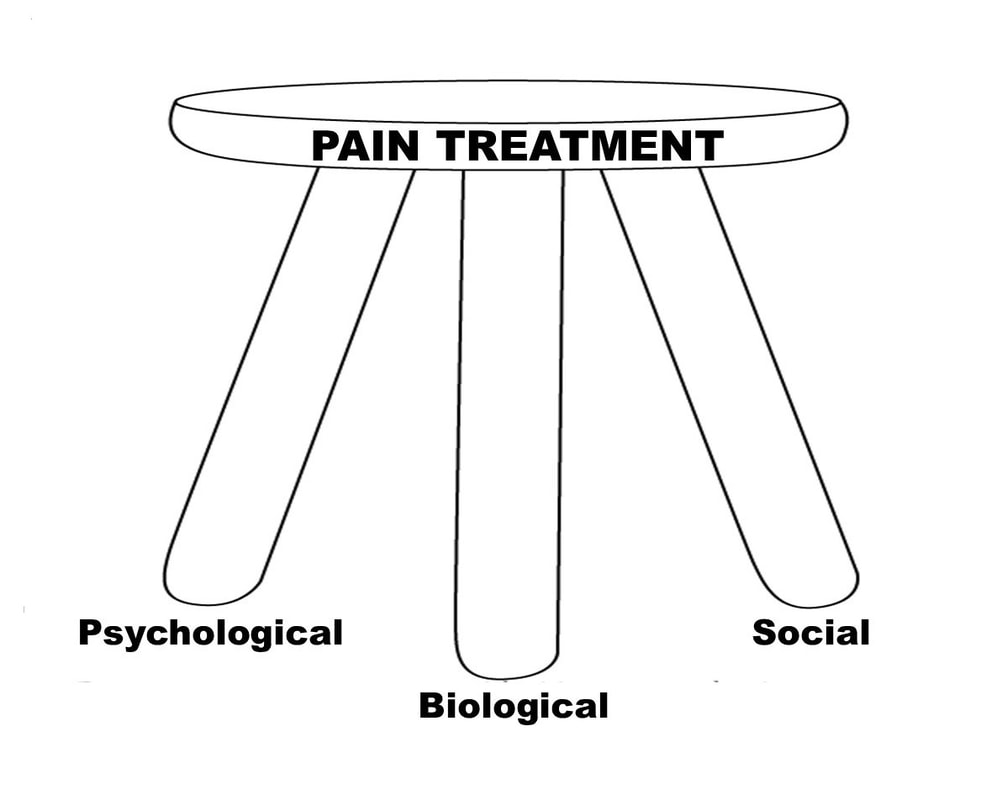
We’re more than our bodies. Yet, we’ve been typically treating chronic pain only from a biological perspective – potentially missing two-thirds of potential pain treatment.
Enter the biopsychosocial (BPS) model introduced by Dr. George Engel in 1977. This model of medicine stresses a holistic look at the experience of chronic pain. It not only looks at the biological factors (injury, tissue damage, etc.) but also how our emotional well-being and our social situation influence how we’re affected by chronic pain. Learn more about the biopsychosocial model:
[Updated 11/18/21]
If you have chronic pain, the answer is probably yes. Central sensitization has been tied to a variety of chronic pain conditions including fibromyalgia, whiplash, shoulder pain, neuropathic pain, chronic fatigue syndrome, non-cardiac chest pain, irritable bowel syndrome, temporomandibular disorders, complex regional pain syndrome, low back pain, osteoarthritis, pelvic pain, and headache. What is it Central sensitization, also called centralized pain, is due to maladaptive neuroplastic changes in the spinal cord and brain. And is associated with the development, maintenance, and amplification of chronic pain. The official definition by the International Association for the Study of Pain is, “Increased responsiveness of nociceptive neurons in the central nervous system to their normal or subthreshold afferent input.” Understanding it - putting it in plain language Chronic pain is an abnormal response and doesn’t improve over time. It can happen long after an injury or illness heals. It can be due to a degenerative disease, like arthritis. It can be neurological. It can also have no known biological cause, as in the case of fibromyalgia and many common low back pain conditions. Once it becomes chronic, pain loses its warning function and becomes its own disease/condition. It changes how the brain processes pain – misfiring nerve signals and continuing to tell the body it hurts. Just like an alarm that goes on and won’t turn off. An overreaction or amplification, of sorts. It gets stuck on high alert and the body learns the pain. And it can happen in all chronic pain conditions, no matter the underlying cause. We may feel it when only lightly touched or bumped. The pain can move around to different areas of the body other than the spot of the original injury. It can even change the type of feeling we may have like achiness, stabbing, tingling, or burning, for example. Changing it The good news is we can change our nervous system. Central sensitization can be reversed by doing things that promote positive neuroplasticity like changing how we think about pain, react to pain, and manage pain. Best treatment is a biopsychosocial approach, including pain education, physical therapy, cognitive behavioral therapy, pain acceptance, sleep management, and pharmaceutical management. I got a heavy dose of all these at the Mayo Clinic Pain Rehabilitation Center. Learn more
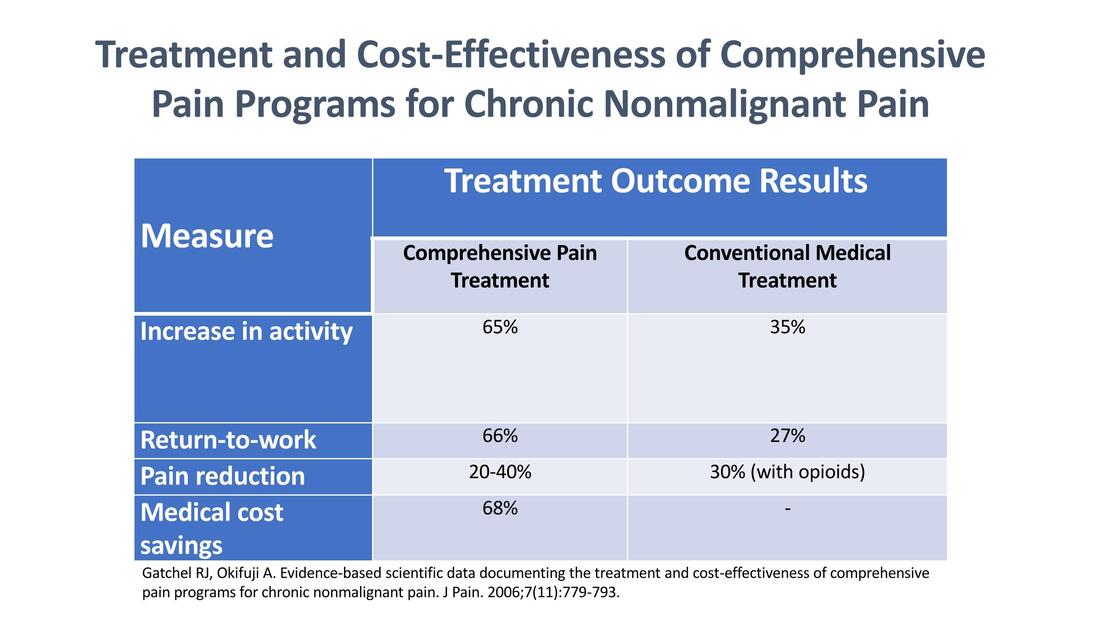
Self-management calming tools Studies have shown that comprehensive (interdisciplinary/multidisciplinary) pain treatment that addresses the biopsychosocial aspects of the chronic pain experience is not only more clinically effective than conventional medical treatment by itself, it’s also more cost-efficient.
It’s no wonder the International Association for the Study of Pain (IASP), the National Academy of Sciences, and the US Pain Management Best Practices Inter-Agency Task Force all recommend comprehensive treatment for chronic pain. I was blessed to be able to attend the Mayo Clinic Pain Rehabilitation Center in Rochester Minnesota - not just once, but twice. I highly recommend the program to anyone interested in talking an active role in managing their own care. It was a life changer for me. Read about my time at Mayo Clinic. Other programs are available. I've included some of them in the Resources tab of this website. Learn more: To better understand the biopsychosocial model of pain and how it affects you...ask questions10/24/2020
You could me missing out on two-thirds of your potential pain treatment. Get the whole story.
|
WelcomeChronic Pain Champions is an information resource/blog/support group to help people living with nonmalignant pain, their families and friends, as well as healthcare professionals. Learn more about this site and the author. Archives
January 2022
Categories
All
© 2021
Tom Bowen Chronic Pain Champions |