|
Changing how you think about pain can change how you feel.
Negative thinking increases focus on the pain, reinforces it, and can actually make the pain feel worse. All while zapping needed energy supply.
Get replacement thought examples here https://www.chronicpainchampions.com/uploads/1/2/0/4/120442940/replacement_thought_examples.pdf P.S. A BIG thank you to all the members of the Chronic Pain Champions Facebook support group who helped contribute to these examples! When pain doesn’t get better and becomes chronic, it’s easy for the pain to become the focus of our lives and we can become paingry.
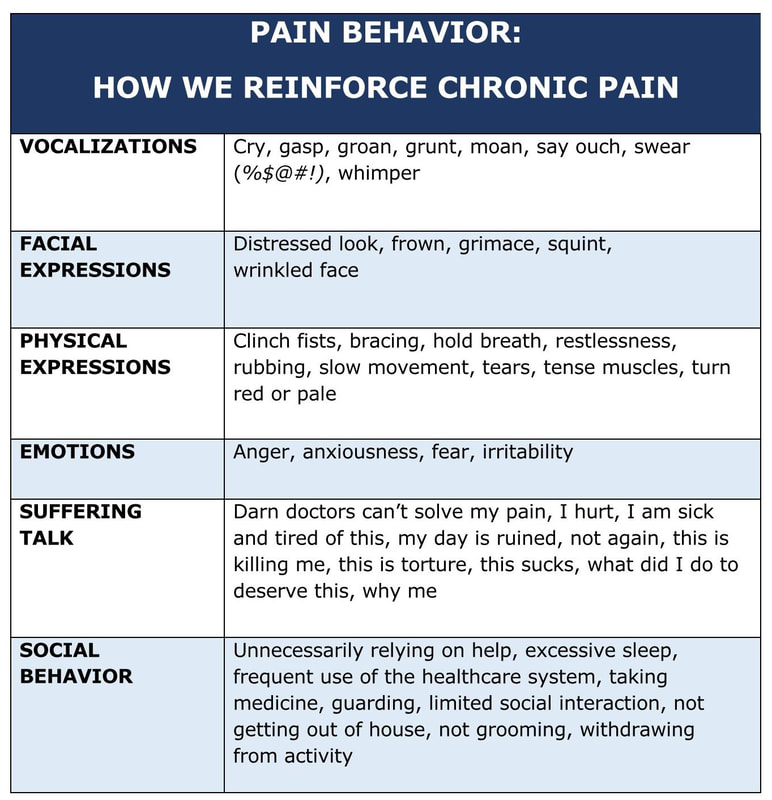
Control anger before it controls you. Tips from the American Psychological Association: https://www.apa.org/topics/anger/control.  What do you do and say when you hurt? How do you react to chronic pain? You may moan or groan. You may make a face and grimace or wince. You may touch or rub the area that hurts. You may stop what you are doing and limit activity. You may even say a few choice words. The body’s natural vocal, verbal, physical, emotional, and social reactions to pain are called pain behaviors. They are our ways of expressing we are hurting. While fine for acute pain like touching a hot stove, these pain behavior reactions place undue focus on chronic pain and reinforce the pain – causing emotional distress and anxiety. Which can lead to reduced coping skills, intensified perceived pain, disability, and increased use of the healthcare system. But, wait, Tom. Are you reinforcing the pain by the sheer fact of talking about it in this article? No. Not really. It is okay to talk about chronic pain in a general or educational sense just like we do any other topic in a conversation. Our emotions stay in check. What is not okay is “stinking thinking” – verbally expressing pain, complaining about it, wallowing in it, or placing blame for it. Pain is a learned response not just a physical problem Research has shown as pain conditions become chronic, the relationship between pain severity and pain behavior weakens. In other words, pain behaviors can become over-exaggerated responses to the pain. Rubbing the spot where it hurts may help you feel better. But what does rubbing and other pain behaviors tell your brain? They tell your brain how to react the next time you have pain. You not only learn the pain; you learn the reaction. And what do pain behaviors tell others around you? How do they react to your demonstrations of pain? They may become confused, over helpful, over cautious, or over critical. They may even stop interacting with you. Change how we react to chronic pain We know what to expect from our pain by the very nature of it being chronic. It is not like twisting an ankle or getting stung by a bee. Below are a few tips to reduce pain behavior:
While easier said than done, these tips can work with practice  Think of pain management as a three-legged stool. Each leg represents one of the three components of pain: biological, psychological, and social. All three components are important to treatment. If one or more of the legs is missing, the stool will topple. And treatment won’t be as successful. Read the whole story: https://www.practicalpainmanagement.com/patient/chronic-pain-biopsychosocial-model also
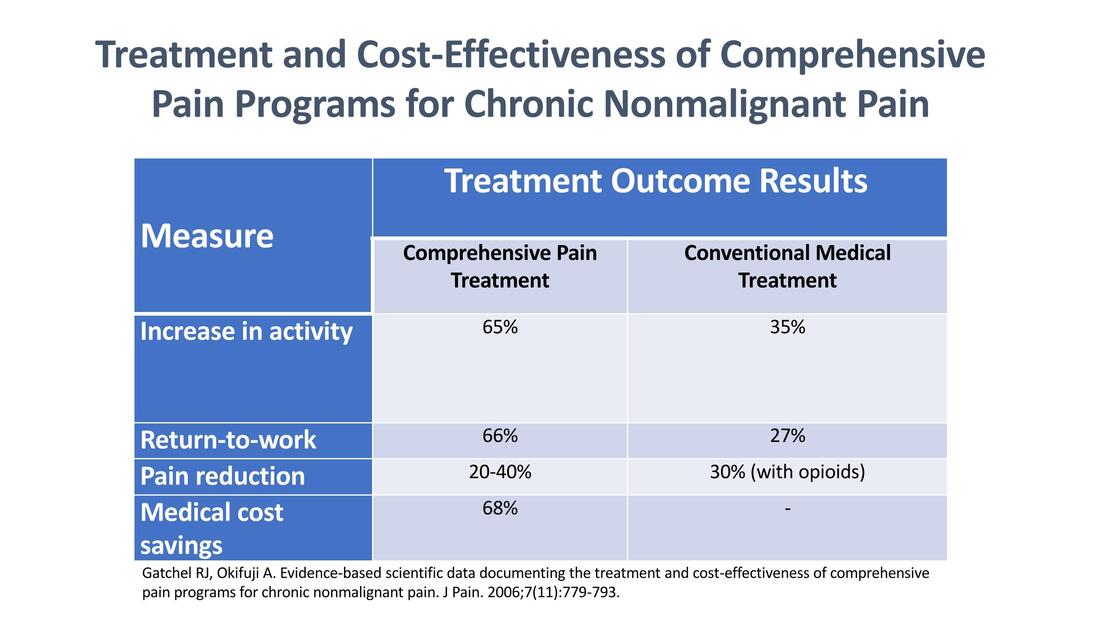
Pain rehabilitation goes beyond medicine and medical interventions – and crosses different disciplines. It doesn’t just focus on removing the pain. It focuses on the patient and how they can play a role in their own pain management. It’s a proven approach – benefiting patients while reducing costs and reliance on the medical system. Having gone through the 3-week outpatient Mayo Pain Rehabilitation Center, at the recommendation of both my family doctor and a general surgeon, I can personally attest to the value of a comprehensive interdisciplinary approach to pain rehabilitation. Do I still have pain? Of course, I do. But I’ve learned to live, despite the pain. Read about my Mayo experience. Major pain rehabilitation programs are also available at Cleveland Clinic, John Hopkins, and Stanford. Links to these programs are provided here. Local and regional programs may also be available. If you don't have access to a formal pain program, talk to your doctor about expanding your pain management team in smaller ways, such as by getting a referral for a psychologist, a physical therapist, or other types of providers that you both feel may be helpful. While cost and insurance coverage may be a concern, expanded care is worth looking into and, in some cases, advocating for to get the best overall outcomes. Learn more about pain rehabilitation. |
WelcomeChronic Pain Champions is an information resource/blog/support group to help people living with nonmalignant pain, their families and friends, as well as healthcare professionals. Learn more about this site and the author. Archives
January 2022
Categories
All
© 2021
Tom Bowen Chronic Pain Champions |